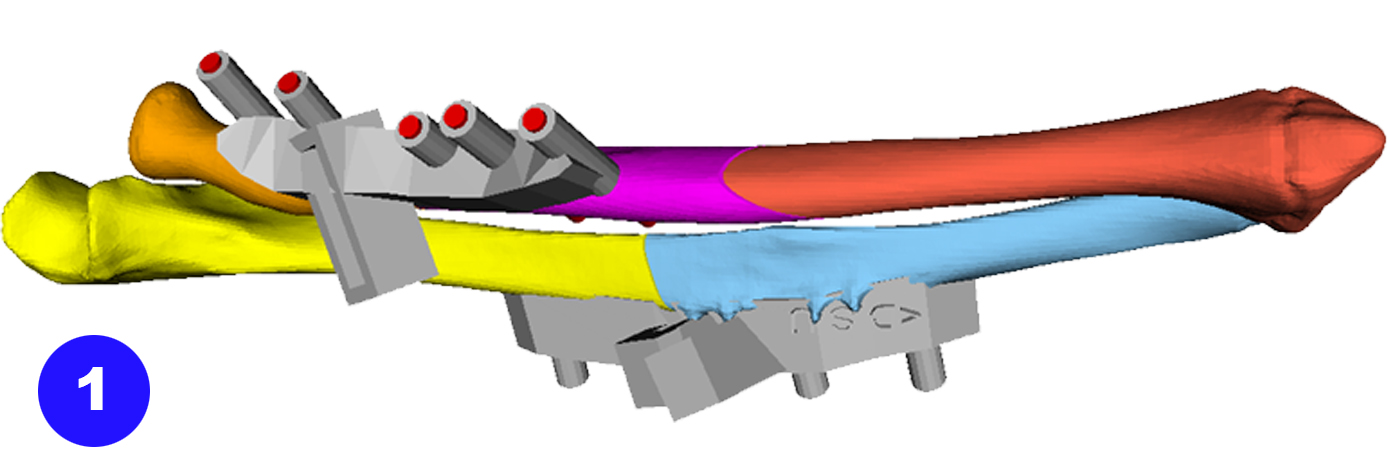
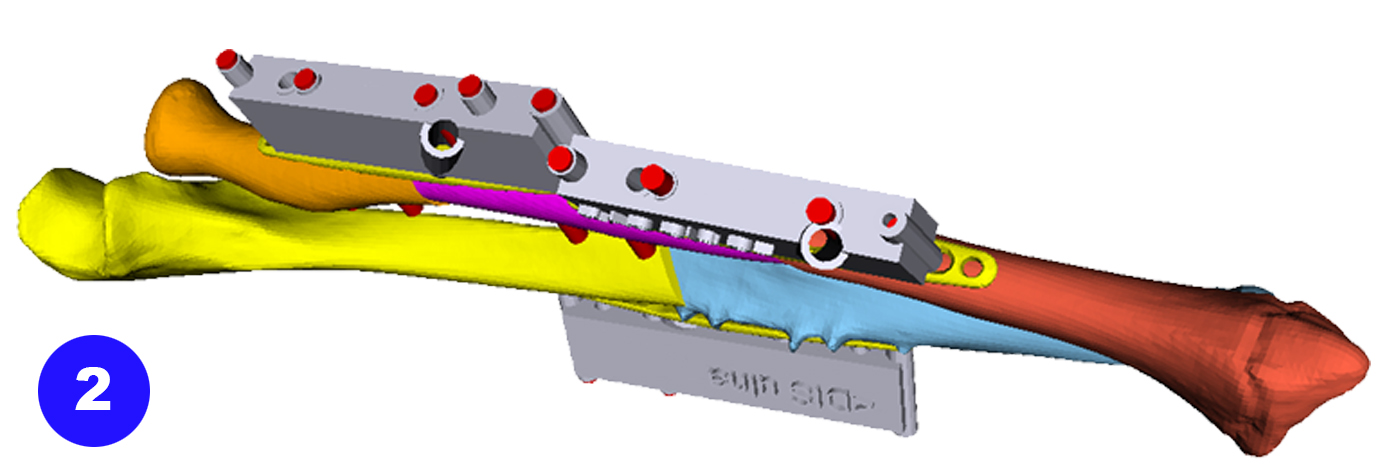
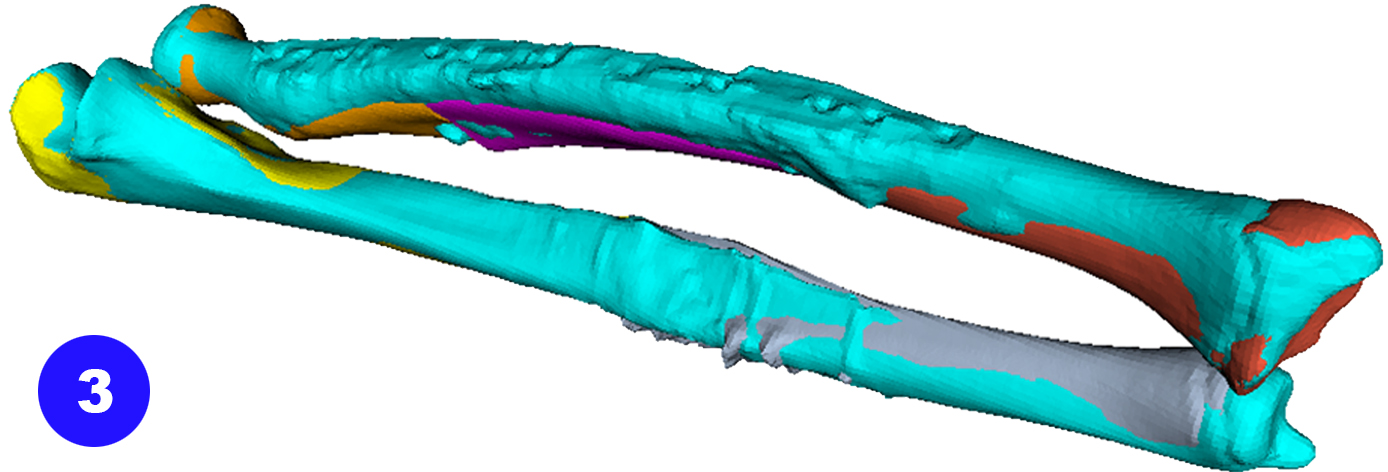
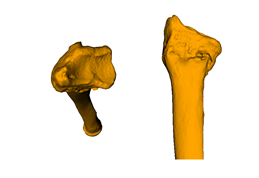
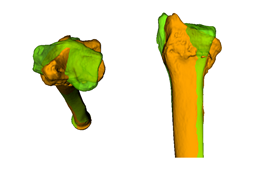
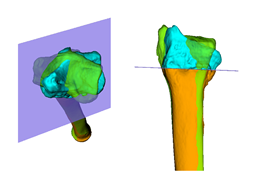
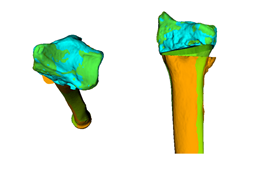
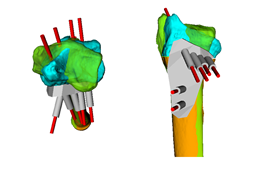
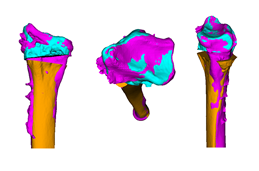In younger and active patients
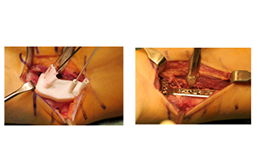
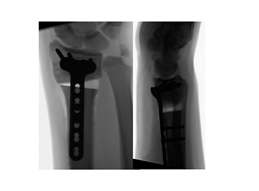
corrective osteotomy
is the preferred treatment option to correct severe bone deformities, because
the function can be restored.
UNDERSTAND OSTEOTOMY
HAVE A QUESTION?
LOGIN